On September 30 when I went in for my 39 week visit the nurse was taking my blood pressure and we started talking about possible induction dates, given that I was 39 weeks and had made zero progress. The baby was still relatively high, my cervix was "semi-firm" and I hadn't dilated at all. I was talking about wanting to wait until after Yom Kippur on the 8th and the nurse looked at me and said "I think today is a great day for an induction."
"Not today!" I said. "Let's at least wait till after the due date."
That's when the nurse informed me that my blood pressure was 150/90. Prepregnancy my blood pressure was usually 106-110/65. During pregnancy it's been around 116/75. This jump in blood pressure worried my doctor. She wanted to send me in for an induction since I was so close and she was afraid I was developing pre-e. But because my cervix was totally not ready for labor she sent me to triage for some tests and monitoring.
We went home, grabbed my hospital bag and packed a separate bag with movies, my computer, and magazines, just in case I was going to get induced. We knew we'd be in for a long induction if that were the case. We grabbed some dinner on the way to the hospital for the same reason.
All my tests were fine. I had no swelling, vision changes, no headaches. There was no protein in my urine and no indication of anything going on with my liver or kidneys. But my blood pressure was staying in the 130s so they decided to admit and induce.
As an aside, Friday night my blood pressure dropped back down to where it usually is, 106-110/65.
The oncall doctor flat out said to me "I wouldn't want to be induced if I were you either. Not with such an unfavorable cervix. Right now your chances of a C-section are 50%." But I have to say, all the health care professionals I came across were ridiculously kind, supportive, and wonderful. I was told multiple times they did not want to do a C-Section on me and we could keep the induction going as long as it took. In fact, the oncall doctor told me they'd start me on Cytotec to soften my cervix and Saturday morning they'd bring me breakfast before starting Pitocin.
They applied the first Cytotec and four hours later my cervix was still semi-firm but I was dilated to 1 cm. So they applied another Cytotec and we waited another four hours. And this time there was no change. The nurse didn't feel like things were progressing, but the on call doctor was encouraged by the dilation and wanted to start the pitocin right away. No breakfast for me!
They started the pitocin and for 12 hours we waited. At this point I was having contractions back to back, less than a minute apart, but it just felt like menstrual cramps since they weren't strong enough to be really doing anything. In fact, after those 12 hours there was still no cervical change. By this time I had been in the hospital for 24 hours.
The newest oncall doctor came in to talk to me about breaking my water. I wasn't really receptive. I told her I was worried that was going to put me on a timeline for a C-section since I needed to get the baby out in 24 hours. Once again, I was assured there was no timeline. I was hooked up to monitors and in the hospital and as long as I was okay and the baby was okay there was no need to rush into a C-section after 24 hours. Plus they would do everything possible to avoid infection by not doing checks unless necessary. And so they broke my water. Which was really uncomfortable.
Those back to back contractions? Now they were starting to feel like something and I couldn't even get a breather between the end of one and beginning of another. So I got my first epidural. Which worked great for about 3 hours - perfect. I could feel and move my legs, toes, everything - just not the contractions. To be fair though, they were having trouble monitoring my contractions too. And the baby's heart rate was staying nice and strong - but not accelerating or decelerating. By this time I was on the third oncall doctor who wanted to insert an interuterine pressure catheter to keep an eye on the baby and the contractions. Thatboy was not happy about this. He pointed out they were trying to keep any cervical intrusion to a minimum to decrease the risk of infection and chance at C-Section. But this doctor wasn't as go with the flow as the others. He felt that I really wasn't making any progress and if I had my way I'd still be waiting to have the baby on Monday. Luckily the baby's heart rate started showing accelerations and the pressure catheter was deemed unnecessary.
Shortly after that conversation I started feeling my contractions again. First as mild pressure, then as full on contractions. I'd pressed the "more more more" button to the max and no relief. The anesthesiologist attempted to put in another bolster of the drug into my epidural. No go. He decided the catheter must have moved in the space and wasn't hitting the window it needed to, so he was going to have to redo it. After the second epidural they checked me and I was at 7 cm.
They got the room ready for me to push since I gone from 0 to 60 in about 3 hours. They called the negative oncall doctor and told him not to go back to sleep. He came in to check on me quite surprised. "Guess this baby wanted to prove you wrong." I told him.
They let me rest and told me to let them know when I started to feel the urge to push. When I called them back in about 40 minutes later I was at 9.5 cm. They decided to let me "labor down" to 10, but then the baby's heart rate started decelerating down to the 50s with every contraction. It would go right back up, but was being fairly consistent and they felt that I was a good pusher and could probably overcome the fact he hadn't reached pushing station. So they got everything set and I was now at 10 cm anyway so we were on our way.
They set up the squatting bar onto the bed and tied a sheet on the middle. With each contraction I pulled myself up the sheet as though I were climbing a rope as I pushed. The second epidural had started to wear off at this point, so I was feeling that pressure feeling every time I had a contraction. At this point I didn't mind because it helped me know when to push.
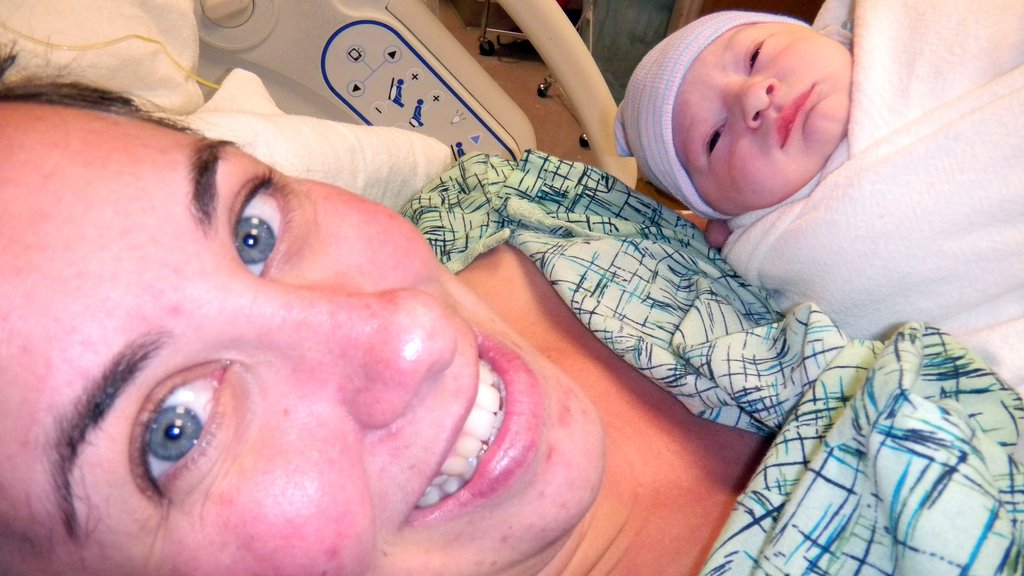
40 minutes later, at 2:42am on October 2, Thatbaby made his way into the world with his cord wrapped around his neck twice. NICU was there because of the decels and because of some meconium present in my bloody show so he was taken over by them for some aspiration. With everything that was going on, we didn't even know the sex of the baby so I sent Thatboy over to the NICU team to check it out. Thatbaby was a boy!
He weighed 7lbs 6.5 oz and was 20 inches long. He scored an 8/9 on his apgar.
Thatbaby was placed on my chest for some bonding and feeding while the doctor delivered the placenta and sewed me back up. By this time the epidural had worn off again and the sewing me back up part was really uncomfortable and felt like it took forever!
During the "recovery" period, Thatbaby's respiration was a little fast. They checked his oxygen saturation which was fine, but they wanted to keep an eye on his breathing, just in case. They brought us up to the post partum floor and Thatbaby was taken to the Observation Unit for pretty much that - observation. Thatboy and I used the time to get some sleep and a couple hours later our little boy was brought back to us.
We spent the whole day in the hospital "recovering" which really wasn't bad at all. Because Thatbaby was taken to the IOU my chart had us marked down as a "separation" and I got an extra visit with a lactation consultant. Which was nice because Thatbaby wasn't a huge fan of breast feeding at first. He didn't like having to do work to eat - which is proof he takes after his father. He would latch on, then look up at me like - "Okay I'm here, now what?"
I didn't have any sort of post partum pain or severe bleeding so we got the okay to be discharged the next day.






Oh my goodness. I can't believe you had to drive home in those conditions. The first ride is nerve-wracking enough. Thank you for sharing your beautiful birth story. I loved reading it.
ReplyDeleteI'm SO glad you shared this!! I love reading birth stories even though I'm sans baby. Somehow it just makes me feel more prepared for the eventual "someday"!
ReplyDeleteI'm a sucker for birth stories! I wrote out mine, thinking I would blog about it...but never ended up doing anything with it.
ReplyDeleteMy son was supposed to come 3 weeks later but he was in hurry to be born! It was a very easy labor and even doctor couldn't believe how quick this was going to be!
ReplyDelete